Get your motherhood essentials
in 3 simple steps
- Provide your insurance information
- We verify your coverage and submit all required paperwork on your behalf
- Choose from the curated breast pumps, pregnancy support and postpartum recovery items covered by your insurance
congrats!
We ship them free, straight to your door.





What Our Patients Are Saying


Pregnancy Support
You’re glowing, mama. And growing, too! You may experience symptoms such as back pain or swelling. Pregnancy support can help to provide relief.


Postpartum Recovery
Whether you have a vaginal or c-section delivery, these items help to speed up your recovery and facilitate healing.
Most Popular
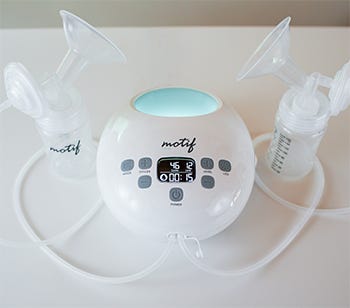
Breast Pumps
As Seen In




Motherhood Through Insurance
Congratulations on your growing family! We understand how much work goes into preparing for a new baby. Our goal is to make it easy for you to get the supplies you’ll need for this exciting stage of life.



Support
Pregnancy support redistributes weight for incredible relief and comfort during pregnancy.


Recover
Postpartum recovery garments can be worn up to four months after birth to speed up the healing process and address issues such as diastasis recti.

Getting a Breast Pump
To qualify for your breast pump through insurance, simply fill out our Qualify Form and a Breastpump Specialist will contact you in 1-3 business days to discuss your coverage options and eligibility. The process is so easy — you will be on the way to receiving your free breast pump through your insurance provider in no time.
You can also purchase a breast pump and any additional supplies that you might need during your breastfeeding journey. Choose from top brands and a variety of breast pumps all offered at a low price. Even better, shipping is free on all orders over $49!
Finding the Right Breast Pump
Aeroflow Breastpumps is here to help you find the best breast pump to accompany you during your experience as a new mom. Our team of dedicated Specialists will be there for you through the whole process and can answer any questions that you have along the way. To find the right breast pump for your lifestyle, start by browsing our selection of name brand pumps to decide which features you need. You can also read more about each pump on our helpful brochures attached to each pump or consult our blog to find out more about how breast pumps work.
Hospital Grade Breast Pumps
A hospital grade breast pump is a multi-use rental breast pump designed for mothers with medical issues preventing them from properly breastfeeding their babies, or for mothers of babies with genetic issues in the NICU. A hospital grade breast pump is a multi-user rental breast pump with a stronger strength suction, special wavelength, and programming that allows mothers with certain medical necessities to produce the maximum amount of breast milk possible.
Aeroflow Breastpumps is able to help moms rent hospital grade pumps; however, a prescription from your physician is required with a corresponding diagnosis code. To inquire about renting a hospital grade pump through insurance, call us 844-867-9890 and a Breastpump Specialist will work with you to collect the necessary insurance and prescription information.


Our systems are currently down, but we have your information and will contact you shortly.



